Remote Contrast Coverage Incident Escalation: Roles, Responsibilities and Timelines


Key Takeaways
- Remote contrast supervision requires a structured, tiered escalation protocol. Without one, response times slow down, and patient safety is compromised.
- Onsite staff and remote radiologists each carry distinct, non-overlapping responsibilities during a contrast incident that must be rehearsed and clearly documented.
- ACR and CMS compliance standards require real-time audio-video connectivity, onsite BLS certification, and the availability of emergency medication during all remotely supervised contrast procedures.
- The first two minutes of a contrast reaction are the most critical, and what onsite technologists do before the remote radiologist can direct care often determines patient outcomes.
- At ContrastConnect, our qualified radiologists manage 5–10 contrast reactions daily across 55,000+ monthly exams, with documented zero missed responses. We deliver the escalation expertise, audit-ready documentation, and HIPAA-compliant connectivity your facility needs to stay compliant and fully operational without adding onsite staff.
When a Contrast Incident Happens Remotely, Every Second Counts
Unlike traditional in-person supervision, remote contrast coverage introduces a physical gap between the directing physician and the patient. That gap does not reduce safety, but it does change how escalation must be structured.
Every action taken relies on clear communication, and every second of delay is a second the patient waits. This is why escalation in remote contrast coverage requires a precision coordination system with defined roles, timed checkpoints, and clear decision trees.
The onsite technologist acts as the first responder, responsible for managing the physical environment. Meanwhile, the remote supervising radiologist assesses the situation in real time via audio and video to provide clinical decision-making.
The escalation timeline ranges from 2 to 10 minutes, each with a different framework to help manage contrast incidents effectively.
Understanding the tiers of remote contrast incident escalation and their strict timelines is critical to safely managing adverse outcomes.
The Three Tiers of Remote Contrast Incident Escalation
Effective escalation moves through three distinct tiers, each triggered by the severity of the situation and the response capacity at each level.
Tier 1: Onsite Technologist Response
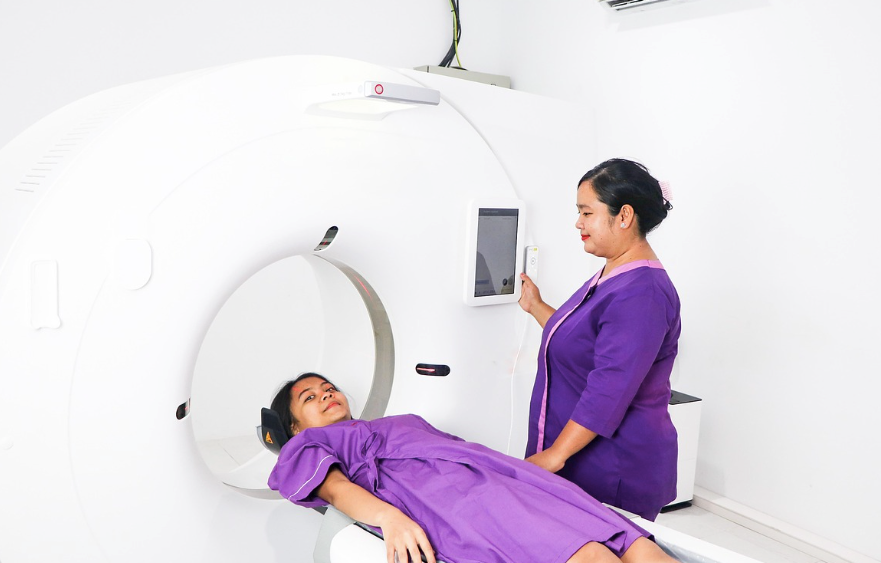
The moment a contrast reaction is observed, Tier 1 activates. This tier is entirely the onsite technologist's responsibility. Their job in these first critical moments is to stop the contrast injection, assess the patient's condition, and initiate the facility's emergency response checklist.
Onsite technologists must be trained to recognize contrast reactions and categorize them quickly. A mild reaction, such as flushing, nausea, or mild urticaria, requires monitoring and physician notification. A moderate reaction, such as significant urticaria, bronchospasm, or mild hypotension, requires immediate administration of medication per standing orders.
A severe reaction, such as anaphylaxis, loss of consciousness, or cardiovascular compromise, requires simultaneous activation of emergency services and direct real-time direction from the supervising radiologist.
Tier 2: Remote Supervising Radiologist Escalation
Once the onsite technologist has initiated contact, the remote supervising radiologist assumes responsibility for clinical decision-making.
The remote physician assesses the situation via real-time audio-video, asks targeted questions about the patient's presentation, and issues specific treatment instructions in accordance with the ACR Manual on Contrast Media protocols. At this tier, the radiologist also decides whether to escalate further.
Tier 3: Emergency Services & Hospital Leadership Notification
Tier 3 is the full-system response. Emergency services are called, the facility's emergency action plan activates, and hospital administration or the on-call medical director is notified. The remote radiologist remains on the audio-video connection, continuing to direct care until emergency responders take over or the patient is stabilized.
Documentation begins at Tier 3 even while the incident is still active. Staff must record the time of reaction onset, the time each escalation tier was activated, treatments administered and by whom, and the patient's response at each interval.
Who Does What: What Are the Roles in a Remote Contrast Incident?
In a remote contrast incident, three primary roles are involved in the response: the onsite technologist, the remote supervising radiologist, and the facility administrator or charge nurse.
Onsite Technologist Responsibilities
The onsite technologist is the first responder. Their responsibilities during a contrast incident include stopping the injection, activating the communication link with the remote radiologist, assessing and documenting the patient's vital signs, and administering emergency medications per standing physician orders.
They must also manage the physical environment, such as clearing the room of unnecessary personnel, ensuring crash cart or emergency medication kit accessibility, and preparing the patient for potential transfer if escalation reaches Tier 3.
All of this happens while simultaneously relaying real-time updates to the remote supervising radiologist.
Remote Supervising Radiologist Responsibilities
The remote radiologist's role during an incident is command and clinical direction. From the moment the technologist initiates contact, the radiologist must be fully present on the audio-video link.
They assess the patient's presentation through real-time visual and verbal reporting, issue precise treatment instructions, and make escalation decisions at defined time thresholds. They are also responsible for maintaining documentation of their own directives throughout the event.
Facility Administrator or Charge Nurse Responsibilities
The facility administrator or charge nurse operates as the logistics coordinator during a contrast incident. While the technologist manages the patient and the radiologist manages clinical direction, the administrator ensures that the right resources reach the room at the right time.
This means confirming that emergency medications and equipment are accessible and notifying additional onsite clinical staff if needed. It also involves managing communication with family members or patient companions, and initiating the facility's formal emergency action plan if Tier 3 is reached.
Escalation Timelines You Must Follow
The framework below reflects current ACR guidance and CMS virtual supervision requirements, and it is the structure that separates facilities that manage contrast incidents safely from those that do not.
0 to 2 Minutes: Immediate Onsite Response
The onsite technologist owns the first two minutes, which represent the most physically demanding phase of the entire response. The injection must be stopped immediately if an adverse reaction is suspected.
The patient is assessed using the ACR's contrast reaction classification criteria: mild, moderate, or severe. Vital signs are checked if the patient's condition permits, and the emergency communication link to the remote radiologist is opened immediately.
If the reaction appears severe from the outset, the technologist does not wait for the radiologist's direction before calling emergency services. The call goes out simultaneously. Waiting for remote authorization in a life-threatening event costs time the patient does not have.
2 to 5 Minutes: Remote Radiologist Notification and Direction
By the two-minute mark, the remote supervising radiologist must be actively engaged on the audio-video connection. If initial contact attempts fail, the onsite technologist must immediately activate the facility's backup physician contact protocol.
Once connected, the radiologist takes over clinical direction with a structured rapid assessment. They need the following information immediately from the onsite technologist:
- Type and volume of contrast agent administered before the reaction occurred.
- Exact symptoms observed and their onset time relative to the injection.
- Current vital signs: blood pressure, heart rate, oxygen saturation, and respiratory rate.
- Patient's known contrast allergy history and any premedication given.
- Current level of consciousness and the patient's ability to communicate.
- Emergency medications and equipment currently available onsite.
With this information, the radiologist issues specific treatment directives and sets a reassessment checkpoint within 2 to 3 minutes to evaluate the patient's response to treatment.
5 to 10 Minutes: Decision to Call Emergency Services
If a moderate or severe reaction has not shown clear improvement by the five-minute mark, the decision to activate emergency services should already be made. The remote radiologist explicitly directs this call, and the onsite technologist or administrator executes it without delay.
Facilities located more than ten minutes from the nearest emergency response unit carry an even higher obligation to escalate early, since transport time compounds any delay in the activation decision.
Post-Incident: Documentation & Review Requirements
Within 24 to 72 hours, the facility's quality assurance process should examine what happened, whether the protocol was followed, and identify gaps or delays.
Once the patient is stabilized or transferred, the documentation phase begins immediately. A complete incident report must capture the following:
- The time of reaction onset.
- Each escalation action taken and its timestamp.
- All medications administered and by whom.
- The remote radiologist's directives.
- The technologist's responses.
- The patient's condition at each interval throughout the event.
Get Safe Remote Contrast Coverage at ContrastConnect

Even the best-written escalation protocol only works when a qualified radiologist is available the moment it's needed, and for many outpatient imaging facilities, that's exactly where the gap exists. At ContrastConnect, we built our platform specifically to close that gap.
Our qualified radiologists are available through a secure, HIPAA- and HITECH-compliant system that provides immediate, qualified supervision. Our physicians supervise more than 55,000 contrast exams every month and manage 5–10 reactions daily, giving our team a depth of real-world escalation experience that most providers simply don't encounter at that volume.
Every interaction is backed by audit-ready documentation, including discharge summaries, incident reports, and state-specific compliance records aligned with CMS and ACR requirements. If you operate 20 sites or 200+, ContrastConnect gives you a scalable way to ensure every contrast exam has qualified radiologist oversight without adding headcount, extending onsite shifts, or cancelling scans due to coverage gaps.
Start your coverage assessment today.
Frequently Asked Questions (FAQs)
What is the first step an onsite technologist must take when a contrast reaction occurs during remote supervision?
The first step is to stop the contrast injection immediately, even if the reaction is mild or unconfirmed. The next immediate action is to open the audio-video communication link to the remote supervising radiologist while simultaneously assessing the patient's symptoms and vital signs.
What happens if the audio-video connection fails during a contrast incident?
A connection failure during an active contrast incident is a critical systems failure, and every facility must have a pre-tested backup protocol in place before this scenario occurs. The backup typically involves an immediate switch to telephone communication with the same remote radiologist, followed by parallel attempts to restore the video connection.
If neither audio nor video can be restored within 60 to 90 seconds, the facility's backup physician contact must be reached immediately.
How quickly must a contrast reaction be documented after it occurs?
Documentation of a contrast reaction must begin during the incident, not after it. Real-time recording of reaction onset time, observed symptoms, treatments administered, and the remote radiologist's directives should begin as soon as a second staff member can take over documentation duties.
A formal written incident report must be completed before the end of the shift in which the reaction occurred.
What certifications must onsite staff hold during remotely supervised contrast procedures?
At a minimum, at least one onsite staff member present during every remotely supervised contrast procedure must hold a current Basic Life Support (BLS) certification. Many facilities and their credentialing standards also require that contrast-administering technologists hold advanced certification in contrast media administration, such as that offered through the American Registry of Radiologic Technologists (ARRT) or equivalent state-recognized programs.
What sets ContrastConnect apart from other remote contrast coverage providers?
At ContrastConnect, our radiologists supervise more than 55,000 contrast exams monthly and manage 5–10 reactions daily, delivering a depth of clinical experience most providers can't match. Additionally, every session is fully documented with audit-ready incident reports, discharge summaries, and state-specific compliance records aligned with CMS and ACR requirements.
*Note: Information provided is for general guidance only and does not constitute medical, legal, or financial advice. Pricing estimates and regulatory requirements are current at the time of writing and subject to change. For personalized consultation on imaging center operations and virtual contrast supervision, contact ContrastConnect.
Trusted Nationwide








































.avif)











.avif)











.avif)




1,000,000
Contrast exams supervised annually
75,000+
Hours of supervision monthly
3,900+
Technologists certified
100s
Of imaging partners nationwide
130+
Contrast reactions treated monthly
100%
Requested hours covered
Connect with us.


