Remote Contrast Supervision & Radiology Shortages: 2026 Industry Impact


Key Takeaways
- The U.S. faces a projected shortage of 17,000 to 42,000 specialists, including radiologists, by 2033, according to the Association of American Medical Colleges (AAMC), and rural imaging centers are already feeling the strain.
- The Centers for Medicare & Medicaid Services (CMS) permanently authorized virtual contrast supervision starting January 2026, eliminating the requirement for on-site radiologists at qualifying outpatient and rural facilities.
- Remote contrast supervision allows a single radiologist to oversee contrast-enhanced procedures across multiple sites in real time using secure audio/video technology.
- Facilities that adopt virtual supervision platforms now will be better positioned to maintain imaging access, reduce patient transfers, and control costs as workforce pressures intensify through 2026 and beyond.
- At ContrastConnect, we provide immediate, seconds-based physician response through live audio and video connection. As a radiologist-owned platform, we provide underserved imaging facilities with on-call radiologists who can evaluate contrast reactions and guide technologists in real time.
Is There a Radiologist Shortage?
Two forces are reshaping the imaging industry in 2026: a deepening radiologist shortage and the permanent CMS authorization of virtual contrast supervision that took effect in January.
Outpatient and rural facilities that can no longer rely on a full-time on-site radiologist now have a regulatory path to compliant remote coverage, and they need it urgently. Hiring cannot keep pace with imaging demand, and the cost of every canceled scan, transferred patient, or extended wait time falls directly on already stretched centers.
ContrastConnect and similar virtual supervision platforms are purpose-built to close this gap, providing live radiologist oversight through a HIPAA-compliant audio/video connection. Alternatives such as locum coverage or aggressive in-house recruitment rarely match the speed, scalability, or unit economics of a dedicated remote supervision model.
In this guide, we break down the workforce numbers behind the shortage, the shape of the new CMS framework, and the readiness steps imaging leaders should take before 2026 pressures peak.
The U.S. Faces a Deficit of Up to 42,000 Radiologists by 2033
The projected shortfall of 17,000 to 42,000 specialists, a category that includes radiologists, pathologists, and psychiatrists, by 2033, is one of the most significant workforce crises in modern healthcare. Meanwhile, the AAMC's update projects an overall physician shortage of up to 86,000 by 2036.
Unlike nursing shortages, which draw significant public attention, the radiology gap tends to be invisible to patients until they're told their scan needs to be rescheduled by 3 weeks or that they need to drive 90 minutes to a facility that can perform their contrast study.
Multiple structural forces are converging to create this deficit simultaneously. An aging radiologist workforce is moving toward retirement. Residency program caps limit how quickly new physicians can enter the specialty.
Why Residency Programs Are Not Keeping Pace With Demand
Radiology training takes five years after medical school, a required preliminary clinical year followed by a four-year residency, plus one to two years of fellowship for most subspecialists.
The pipeline is long and capacity-constrained. Residency positions are not infinitely expandable; they require accredited programs, faculty oversight, clinical case volumes, and institutional resources.
Even with modest increases in residency slots over the past decade, the graduation rate for new radiologists cannot keep pace with the accelerating demand or the rate of retirement among experienced radiologists.
This structural lag means that even if every radiology residency program in the U.S. expanded enrollment today, the workforce impact wouldn't be felt until the early 2030s at the earliest. For facilities dealing with staffing challenges right now, that timeline offers no practical relief.
States With the Most Severe Shortages Right Now
While the shortage is national, certain states are disproportionately affected. Oklahoma, Mississippi, Nevada, and Wyoming rank among the states with the most pronounced radiologist deficits per capita.
These states share common characteristics: large, rural or frontier geographies, lower median physician compensation than in coastal markets, and healthcare systems that have historically struggled to recruit and retain specialty physicians.
In these environments, the gap between imaging need and imaging capacity is measured in days-long wait times for routine studies and in patients who forgo recommended imaging entirely because access is simply not available locally.
CMS Made Virtual Contrast Supervision Permanent Starting January 2026
One of the most consequential regulatory changes in recent radiology history took effect in January 2026: the CMS permanently authorized virtual supervision for contrast-enhanced imaging procedures.
This rule change eliminates the longstanding requirement that a supervising physician be physically present or immediately available on-site during contrast administration at qualifying outpatient and rural facilities.
What Level 2 Diagnostic Tests Are Covered Under the New Rule
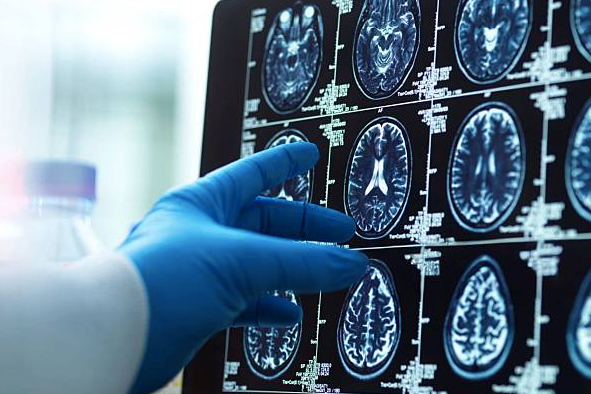
The CMS virtual supervision authorization applies specifically to Level 2 diagnostic tests. This category includes contrast-enhanced CT scans, contrast-enhanced MRI studies, and other imaging procedures that require physician supervision due to the clinical risks associated with contrast agent administration.
Under the previous framework, these studies required a physician to be immediately available in the facility during the procedure. The permanent rule change allows that supervisory role to be fulfilled remotely via real-time audio/video communication, provided the technology meets CMS compliance standards and the supervising physician is actively available throughout the procedure.
Real-Time Audio/Video Requirements Under the CMS Framework
CMS doesn't simply permit any video call to substitute for physical presence. The supervising radiologist must be connected via a HIPAA-compliant, real-time, two-way audio/video link with no perceptible delay that would compromise the ability to respond to an adverse contrast reaction.
The platform must allow the radiologist to both view and communicate with the patient care team in real time. Recorded or asynchronous communication does not satisfy the requirement.
What This Means for On-Site Radiologist Requirements
The practical implication of the CMS rule change is significant: facilities no longer need a radiologist physically inside the building to perform supervised contrast studies.
What they do need is a practicing radiologist who is actively available via a compliant virtual supervision platform during the procedure window; someone who can observe, respond, and intervene in real time if a contrast reaction occurs.
This doesn't eliminate the need for trained on-site clinical staff. Registered nurses, radiologic technologists, and other qualified personnel must remain present to administer contrast, monitor the patient, and follow emergency protocols if directed.
The radiologist's role in the virtual model is supervisory, providing immediate expert guidance and clinical decision-making authority without being physically co-located with the patient.
ContrastConnect is built precisely for this model. Our platform connects imaging facilities with on-call, qualified radiologists who are available in real time via secure audio and video, ready to provide the clinical oversight that CMS now recognizes as sufficient for compliant contrast supervision.
For rural and underserved facilities navigating the new regulatory structure, we offer a practical, immediately deployable solution that closes the coverage gap without requiring a full-time on-site physician.
What Radiology Professionals Should Do Before the 2026 Pressures Peak
The January 2026 CMS rule change has removed a significant regulatory barrier, but adopting virtual supervision still requires deliberate preparation. Facilities that wait until workforce pressures become acute will find themselves implementing new systems under operational duress.
The better approach is to evaluate readiness now, while there's still time to build infrastructure, train staff, and select a supervision platform methodically.
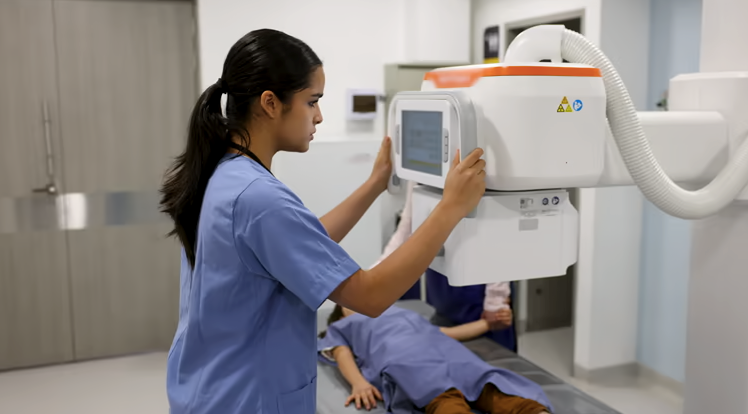
Evaluate Your Facility's Remote Supervision Readiness
- Start with an honest audit of your current staffing model. Map out every contrast-enhanced procedure your facility performs in a given month, identify which of those require physician supervision, and then trace exactly how that supervision is currently being delivered.
- From there, assess your technical baseline against CMS requirements. Run a connectivity audit on your imaging suites. Not just average internet speeds, but sustained upload and download performance during peak operational hours.
- Review your HIPAA compliance posture for audio/video platforms. Survey your nursing and technologist staff on their familiarity with remote communication workflows. The readiness gaps you identify in this assessment will serve as the implementation roadmap for your virtual supervision transition.
Choose the Right Virtual Supervision Platform
Not all virtual supervision platforms are built to the same clinical and compliance standards. Evaluate prospective platforms on five criteria:
- CMS compliance documentation (the platform should be able to provide explicit confirmation that its technical specifications meet virtual supervision requirements).
- HIPAA compliance.
- Response-time guarantees for connecting with a supervising radiologist.
- Multi-site scheduling capability.
- Integration with your existing RIS/PACS infrastructure.
A platform that checks four of five may create compliance exposure or operational friction, undermining the entire model. Ask vendors for documented case studies from facilities with comparable size and patient volumes to yours.
Remote Supervision Is the New Standard, Choose ContrastConnect for Round-the-Clock Coverage

The radiologist shortage is not easing, and the permanent CMS shift to virtual contrast supervision has given imaging leaders a practical path forward. Facilities that build their remote coverage infrastructure now will protect patient access, revenue, and compliance as 2026 workforce pressures intensify.
At ContrastConnect, we deliver CMS-compliant virtual contrast supervision with real-time audio/video, multi-site scheduling, and around-the-clock radiologist coverage backed by SOC2 and HIPAA/HITECH standards. If you want to see how our platform fits your facilities, start your coverage assessment today.
Start your coverage assessment today →
Frequently Asked Questions (FAQs)
What is remote contrast supervision in radiology?
Remote contrast supervision is a model in which an accredited radiologist provides real-time supervisory oversight of contrast-enhanced imaging procedures from a location outside the facility, using a HIPAA-compliant live audio/video connection. The radiologist monitors the procedure, remains immediately available to respond to contrast reactions, and directs the on-site clinical team throughout the supervision window.
Is virtual contrast supervision covered by CMS in 2026?
Yes. Starting January 2026, CMS permanently authorized virtual supervision for Level 2 diagnostic imaging procedures, including contrast-enhanced CT and MRI studies. This rule change removes the requirement that a physician be physically present or immediately available on-site during contrast administration at qualifying outpatient and rural facilities, provided supervision is delivered via a real-time, HIPAA-compliant audio/video platform that meets CMS technical standards.
Can one radiologist really supervise multiple sites at once?
Yes, with one important clarification: not simultaneously in the literal sense, but concurrently within a well-structured scheduling framework. A single radiologist working within a virtual supervision network can cover multiple facilities during the same shift by staggering procedure windows so that active supervision periods do not overlap.
What equipment does a facility need for virtual contrast supervision?
The core technical requirements are more accessible than most facilities expect. At minimum, you need a stable high-speed internet connection with sufficient sustained bandwidth in the imaging suite itself, a HIPAA-compliant audio/video platform, a dedicated monitor, tablet, or secure workstation. They must all be positioned to allow the on-site team to communicate with the remote radiologist without disrupting the procedure workflow.
What are the typical response times at ContrastConnect?
At ContrastConnect, we operate on a seconds-based response model, meaning the moment a technologist flags a contrast reaction, an on-call physician is connected live via audio and video almost instantly. From there, the physician assesses the patient's symptoms and vitals in real time and directs the technologist on exactly what to do next. We actively track and measure response times to ensure no reaction ever waits longer than necessary for expert medical guidance.
*Note: Information provided is for general guidance only and does not constitute medical, legal, or financial advice. Pricing estimates and regulatory requirements are current at the time of writing and subject to change. For personalized consultation on imaging center operations and virtual contrast supervision, contact ContrastConnect.
Trusted Nationwide








































.avif)











.avif)











.avif)




1,000,000
Contrast exams supervised annually
75,000+
Hours of supervision monthly
3,900+
Technologists certified
100s
Of imaging partners nationwide
130+
Contrast reactions treated monthly
100%
Requested hours covered
Connect with us.


